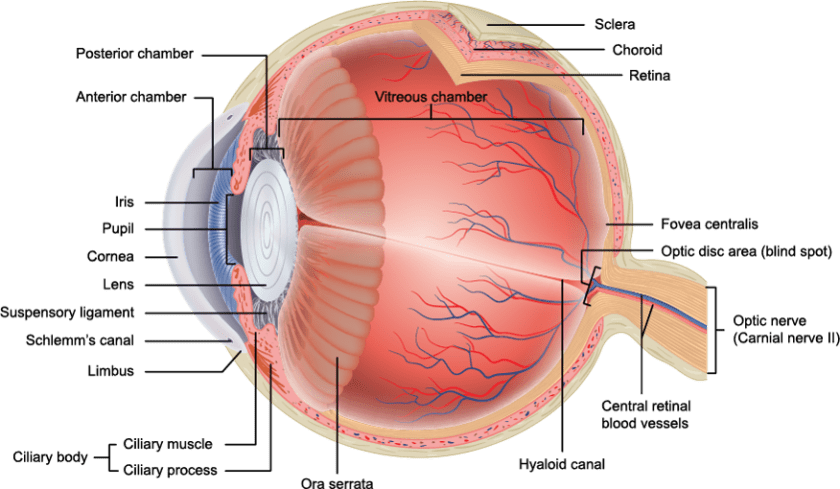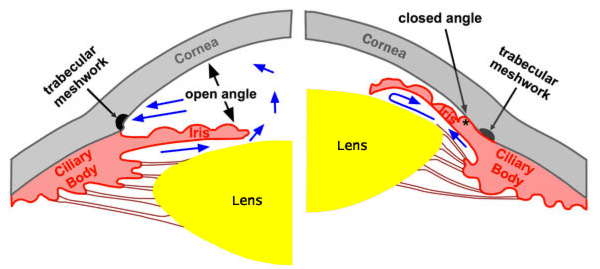
The front of the eyeball is filled with a colourless fluid, known as aqueous humour. It is continually being produced in the eye and drained from the eye, through a drainage channel in the eye called the trabecular meshwork. In some patients, the part of the eye where the trabecular meshwork is located (known as the angle) is narrow, which can reduce the drainage of fluid from the eye. When pressure builds up in the eye as a result of this, angle closure glaucoma results.
Pressure build up can occur acutely, and can build up to very high levels. This results in symptoms of eye pain, redness, blurred vision and headache. The patient may also experience nausea and vomiting.

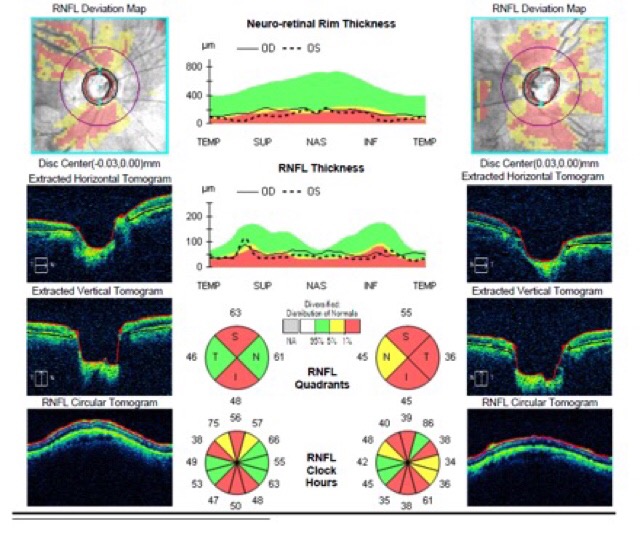
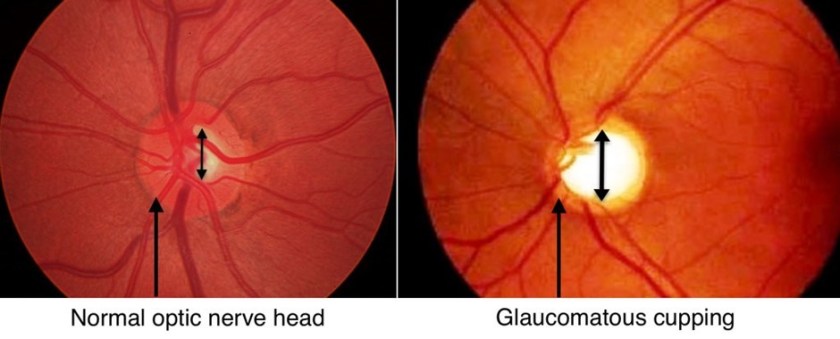
Angle closure glaucoma is an emergency. When the eye pressure is dangerously high, the optic nerve located at the back of the eye can become damaged. This damage is permanent and irreversible, and the patient can permanently lose vision as a result.
How is this condition treated? In the acute situation, the priority is to lower the eye pressure as quickly as possible, to reduce the damage to the nerve. This is achieved using medications, which are administered as eyedrops, oral pills or even injections.
Once pressure is controlled, laser treatment is performed to create an alternative channel for fluid to flow, and prevent the build up of pressure from occurring again.
Patients with this condition sometimes suffer damage to the trabecular meshwork as a result of the high pressure, which results in chronic angle closure glaucoma. These patients often require life long treatment with anti glaucoma eyedrop medications.
Eye pain and redness are symptoms that should never be ignored, especially if they are accompanied by headache and vomiting. If you ever experience these symptoms, consult an Eye doctor without delay.