In Singapore, the overall prevalence of glaucoma is 4%- meaning that in your lifetime, you have a 4% chance of developing glaucoma. Not a big number- the odds are still in your favour, but it is still a condition worth knowing about.
Open angle glaucoma accounts for nearly half of glaucoma in Singapore- 1.7% of the population have or will have this disease. That figure does not sound intimidating. What is worrisome is that this disease does not have many symptoms, and many patients are diagnosed late for this reason.
In open angle glaucoma, the optic nerve at the back of the eye undergoes progressive damage. This is most often (but not always!) due to high eyeball pressure. Contrary to popular belief, this rarely causes pain or discomfort to the eye, and the patient is often unaware that he has glaucoma.
The result of optic nerve damage is visual field loss- reduction in the patient’s peripheral vision. Peripheral vision is important in daily life- it allows us to safely cross roads or drive, for example, but early peripheral vision loss is usually not noticeable. A loss of central vision is noticed by patients immediately, but loss of peripheral vision is much more subtle and can progress to severe loss before it is perceived by the patient.
As a result, open angle glaucoma is often diagnosed late, when significant peripheral field loss has occurred. Occasionally patients present when only tunnel vision remains, or worse, when the peripheral field is completely lost and the disease starts to affect central vision.
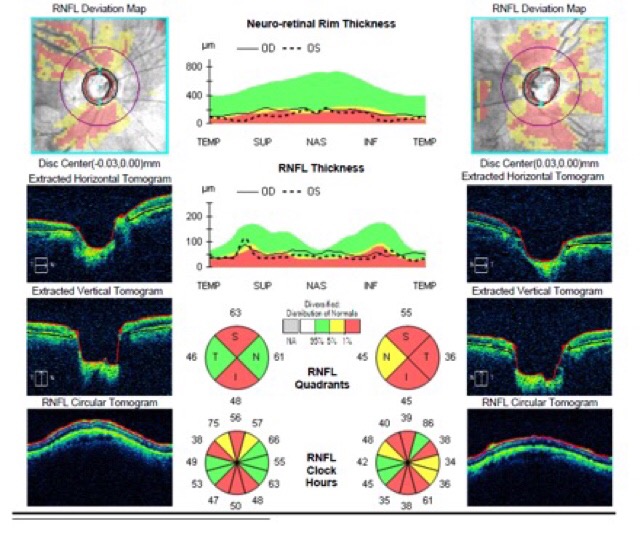
How is open angle glaucoma diagnosed? When patients present to an Ophthalmologist, a detailed history and physical examination is performed. Intraocular pressure is measured- usually raised beyond 21mmHg in the case of open angle glaucoma. Signs that point to the disease- a characteristic weak, thinned-out appearance of the optic nerve, would make one suspicious of the disease. The disease is often confirmed on further testing, where both structure and function of the nerve is tested. High resolution Optical Coherence Tomography (OCT) scans of the optic disc and the surrounding nerve fibre layer can determine if there is any thinning of the nerve due to glaucoma, and Humphrey Visual Field (HVF) testing can map out areas of visual field loss.
How is open angle glaucoma treated? Several eyedrop medications exist that can be instilled to lower intraocular pressure and reduce the progression of nerve damage. If eyedrops are insufficient to treat the disease, laser procedures and surgery can also be done to manage the disease.
If you are over the age of 40, or have a family member who has glaucoma, it is a good idea to go for a comprehensive eye screening to ensure that you do not have this problem.


